Every single day, you potentially face an onslaught of contributing factors that wreak havoc with your complexion and make your adult acne worse.
The four primary acne triggers to be aware of include hormonal imbalance, gut imbalance, stress, and diet.
And the other major contributing factor is this…
Misinformation.
Yep. Inaccurate information that trips up your adult acne care, from commercial skin care companies, dermatologists, Big Pharma, and other professionals. Faulty information concerning the 3 Biggest Skincare Mistakes that leads you down false paths of hope. Wastes your money and time. And perpetuates your acne.
The 3 Biggest Skincare Mistakes help explain WHY you keep breaking out, no matter what you try or how much money you throw at a remedy.
Before we dig in, let’s do a quick review of what acne ACTUALLY is.
Acne is a genetic condition called retention hyperkeratosis. Here’s how it works:
- Every day a layer of dead skin cells is shed inside the pore. Ordinarily, these dead skin cells are pushed from behind by newer cells rising to the skin’s surface, then flake off in a normal, healthy pore.
- This continuous shedding process goes haywire in people with acne. Acne-prone skin produces up to 5x more dead cells than normal, and the excess dead cells stay stuck on the skin’s surface and clog your pores.
- The resulting plug (known as a microcomedone), when mixed with oil, forms a blackhead. When infected with bacteria, forms a blemish.
TAKE NOTE: Acne forms under the skin for up to 90 days before you see it surface! So even if you started the BEST acne clearing skincare routine in the world TODAY, acne that already started forming today still has to work its way up and out through your skin.
Got it? Awesome.
Now you’re equipped to understand the impact and importance of the 3 Biggest Skincare Mistakes.
Big Skincare Mistake #1 ― Allowing your acne to adapt to your skincare regimen.
When it comes to clearing your skin, doggedly sticking to one skincare regimen or treatment can actually perpetuate your adult acne.
And, just like your muscles will adapt to a new fitness routine within a few weeks and then stop improving, your skin will adapt to a new acne-clearing regimen after 2 or 3 weeks and stop responding.
That’s why the one-size-fits-all remedies, antibiotics, and topical prescriptions you take seem to make a difference for a little while, then stop working. It’s not you, you didn’t do anything wrong. It’s just that your skin has adapted. It’s no longer challenged to react.
Instead, you need to change up your regimen so it improves your skin.
Here’s what this “regimen challenge” looks like.
- Increase concentrations of current beneficial acne treatments and skincare regimens, and/or…
- Vary the frequency of existing acne treatments and/or skincare regimens and/or…
- Introduce NEW products and/or skincare regimens.
Then keep up the regimen challenge for 90 days!
That way, you can (1) clear acne that’s already forming below the surface where you can’t see it, (2) prevent NEW acne from forming and (3) break the acne cycle.
This is how you challenge your skin to ensure your skin continues to stop the formation of new acne and heal what’s already there.
When it comes to successful acne treatment, this strategy is PIVOTAL. In fact, it’s the foundation of our proven 95% success rate with our clients.
It’s also, frankly, almost unheard of outside our doors.
The “experts” out there either ignore or are unaware of this truth—likely because it requires personalization for every individual—which helps explain why so many people continue to needlessly suffer the indignity and pain of acne.
Big Skincare Mistake #2 ― Spot-treating your adult acne after it’s erupted
Do you know the expression “tip of the iceberg”? When it comes to adult acne treatments, no truer words spoken!
So often people get hung up on trying to fix what they see in the mirror. Applying acne-drying topicals to pimples. Scrubbing blackheads. Extracting plugs. Injecting painful cysts. But, like the tip of an iceberg, what you see is only the end result of acne. There’s a much deeper issue to consider.
And while it’s understandable you’d want to speed-heal unsightly blemishes as fast as possible (and there’s a place for this in your acne care arsenal)…
By focusing on spot treatments, you’re failing to address the big problem hiding below your skin’s surface. The actual ROOT cause of your acne.
As you discovered earlier, acne is a genetic skin condition and it forms under the skin up to 90 days before you see it surface.
By only spot-treating what you see on your skin’s surface, you’re never going to prevent or control what’s going on underneath—where the trouble starts. And breakouts will continue to bloom, unchecked, along with your misery.
What to do instead?
If you want to FINALLY break the cycle of your never-ending adult acne, you need to:
- Continually treat and challenge your skin for at least 90 days. And…
- Use your acne products daily on your FULL FACE or LARGE AREAS (such as your forehead or chin) even when you’re NOT breaking out.
That way, pre-acne lurking deeper in the skin can be “dissolved” before it surfaces. And you can help prevent new acne from forming in the first place.
Big Skincare Mistake #3 ― Using pore-clogging ingredients in your products
Did you know? Pore-clogging ingredients lurk in your favorite topical skincare, haircare, makeup, laundry, and other beauty and health products.
They’re even in your topical acne care products.
In fact, almost ALL personal care products contain at least one (if not several) of the 125+ ingredients known to clog pores.
From seemingly harmless flower and fruit-derived ingredients found in nature, to synthetic chemicals found in industrial cleaners, the infiltration is so insidious, we keep a comprehensive list of the worst offenders to help defend our clients.
Here’s the problem.
When pore-clogging ingredients are in the makeup you apply, lotions you slather on, even in your laundry detergents, you’re blanketing your pores and allowing even MORE dead skin cells and bacteria to accumulate. No wonder your adult acne gets worse!
While some of these offending ingredients can be harmful and irritating, others are temptingly healthful.
For example, olive oil, coconut oil, and avocado oil are all highly nutritious and have wonderful moisturizing and hydration benefits. But they’re all highly pore-clogging.
Two other major pore-cloggers are Sodium laureth sulfate (SLES) and its chemical cousin, Sodium Lauryl Sulfate (SLS). Emulsifiers and foaming agents, they’re present in most shampoos, conditioners, soaps, body washes, toothpastes, and household and commercial cleaning products.
To protect your skin and help the healing process, check labels! Do your existing products contain these ingredients? Stop using them. And when you’re shopping, avoid these ingredients in any new products you buy. Our Clove Hill Balancing Lotion is completely free of pore-clogging ingredients, soothing and light weight.
Congrats! You’ve just discovered the 3 Biggest Skincare Mistakes that Aggravate and Perpetuate Your Adult Acne.
Apply the lessons you’ve learned and you’ll be on your way to healing your skin and creating a healthier, smoother complexion.

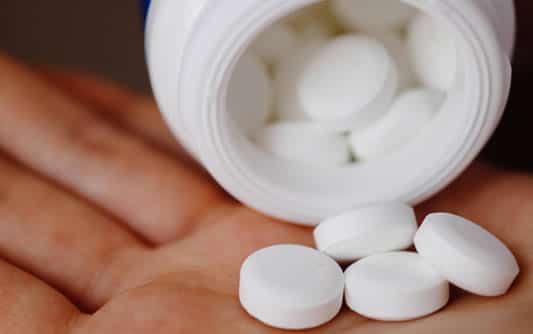
The inexpensive drug could be a safe and effective alternative to antibiotics.
Even though acne is usually at its worst when we’re in our teens and twenties, it’s one of the most common skin conditions in adults, too. As many as one in three women have facial acne in their thirties, and an estimated one in seven continue to struggle with facial blemishes into their fifties.
Many experts recommend considering systemic therapies if topical medications aren’t working or if the acne is causing scars. But that usually means antibiotics, which can be less than ideal for a few reasons.
“Not only is antibiotic resistance a problem, but antibiotics can affect the gut microbiome with unwanted consequences,” says Abigail Waldman, MD, the clinical director of the Mohs and Dermatologic Surgery Center at Brigham and Women’s Hospital and a dermatologist at Mass General Brigham, both in Boston.
For women with a certain type of acne, one alternative has been an inexpensive drug used to treat high blood pressure called spironolactone. Used “off-label” for the skin condition, the drug blocks certain hormones that can cause acne. Men aren’t prescribed spironolactone for acne because of the side effects; men have developed breasts while taking the drug, according to the American Academy of Dermatology.
Largest Randomized Controlled Trial to Look at Spironolactone for Acne
Now results from the first large-scale clinical trial to look at the effectiveness of spironolactone in treating acne, published on May 16 in the British Medical Journal, add support for the inexpensive generic drug.
“Spironolactone has been gaining popularity [as a treatment for acne], and I think this randomized controlled trial with over 400 participants will help. The previous randomized controlled trials were with fewer than 40 women,” says Dr. Waldman, who was not involved in this study.
“Because spironolactone has been generic for many years, there is less financial incentive to conduct large, multicenter placebo-controlled trials in acne patients,” says Lindsay Strowd, MD, an associate professor of dermatology at Wake Forest University School of Medicine and a dermatologist at Atrium Health Wake Forest Baptist, both in Winston-Salem, North Carolina. Dr. Strowd was not involved in the new research.
After 3 Months of Treatment, Women Saw Significant Improvement in Their Acne
The UK study included 410 women older than 18, with an average age of 29, who had acne that had persisted for more than six months, and for whom oral antibiotics would have normally been the next treatment. Half were randomly selected to take spironolactone, while the other half were given a placebo.
For the first six weeks, the spironolactone group took 50 milligrams (mg) a day, and then the dose was increased to 100 mg per day until week 24.
The women were asked to complete questionnaires on their acne and quality of life relating to the condition at the start of the trial and then at 12 and 24 weeks into their treatment.
“The results showed that the women taking spironolactone saw a significant improvement in their acne after 12 and 24 weeks compared to those on the placebo,” said the lead author, Miriam Santer, PhD, a professor of primary care research at the University of Southampton in England, in a press release.
Spironolactone Could Offer an Alternative to Antibiotics for Many Women
“A significantly higher proportion of people also reported that they felt satisfied that their skin had been helped compared with those receiving placebo, and any side effects were uncommon and very minor. These results show that spironolactone could offer an alternative to antibiotics for many women with persistent acne to use alongside topical acne treatments,” she said.
“The findings also showed a significant objective reduction in acne at 24 weeks. This was a well-designed study, and I think it was reassuring that few side effects were noted, with headache being higher in the treatment group,” says Waldman.
What Kind of Acne Responds to Spironolactone?
Spironolactone is used for a very specific type of acne caused by hormonal imbalance in women, says Waldman. “This acne presents on the jawline, neck, and chest,” she says.
Usually, spironolactone is a second- or third-line treatment after topical medications such as benzoyl peroxide, topical retinoids, and oral antibiotics, says Waldman. “Often it is prescribed with an oral contraceptive, which increases its potency and prevents pregnancy complications while on the medication,” she says.
Spironolactone shouldn’t be used during pregnancy or if you’re trying to get pregnant because of its effect on hormones, and so women must be willing to use contraceptives while on the medication, she adds.
Antibiotic Resistance Is One of the Biggest Threats to Global Health
Spironolactone use for acne in the United States is very common, and its popularity has risen as dermatologists have become more conscious of antibiotic resistance. There has also been a push to minimize long-term use of oral antibiotics for acne treatment, says Strowd.
Antibiotic resistance happens when germs like bacteria or fungi no longer respond to the drugs designed to kill them, according to the World Health Organization (WHO).
Antibiotic resistance is one of the biggest threats to global health, food security, and development today, per the organization. Although there are many health situations where antibiotics must be used, it’s important to avoid using them unnecessarily, because it can contribute to antimicrobial resistance.
Contact us today at our Bakersfield dermatology office to schedule an appointment for a acne evaluation.

Familiar Names, Uncommon Condition
Do any of these (somewhat unusual) names sound familiar to you? Humira, Stelara, Cosentyx, Embrel, and Otezla? It’s probably because you’ve seen ads for them. With so many commercials (and celebrities) talking about “clear skin” you might think everyone needs it!
The skin condition those medications, and many others, are designed to treat is psoriasis. It affects 3% of the population, so while we don’t all need it, millions of Americans suffer from it. It’s considered an “immune-mediated disease,” which means a disease with an unclear cause related to the dysfunction of the immune system, according to the National Psoriasis Foundation®.
The Immune System and Psoriasis
Normally, skin cells grow and then fall off in about a month. When you have psoriasis, the immune system doesn’t work properly, causing T-cells to attack the body and prevent skin cells from shedding. Instead of coming off, they pile up in raised “plaques” or scales on the skin.
Don’t Be Fooled by Appearances: The Many Types of Psoriasis
If you think red, itchy, or flaky skin is psoriasis, it might be. But in fact, many skin conditions look similar. That’s why getting an exam from a dermatologist is the quickest way to the best treatment (versus buying an over-the-counter treatment that may or may not treat the outward symptoms).
List of Psoriasis Types
- Plaque psoriasis: Raised, thicker skin in patches, covered with scales; typically on the scalp, elbows, knees, or back.
- Scalp psoriasis: Thin or thick psoriasis on the scalp, can spread to nearby areas like the ears or neck.
- Nail psoriasis: Yellow-brown spots on the nails or tiny potholes, weak or separated nails.
- Guttate psoriasis: Small, scaly spots, often seen in children after an infection like strep throat.
- Inverse psoriasis: Shiny, smooth patches in areas where skin touches skin, like under the arms or in the groin.
- Pustular psoriasis: Painful pus-filled blisters and thicker, scaly skin, often on hands and feet.
- Generalized pustular psoriasis: Rare and serious, shows up as dry, red, and tender skin followed by pus-filled blisters.
- Erythrodermic psoriasis: Life-threatening, noticeable areas of skin that look burned.
What Causes Psoriasis?
While the specific cause is unknown, medical professionals agree it’s genetic. If someone in your family has it, your chances of getting it too are higher. As with many health conditions, you can have a genetic predisposition but never “trigger” the disease itself.
Known Triggers to Avoid
- Stress
- Injuring the skin (cuts, sunburn)
- Infection
- Certain medications, including lithium, prednisone, and hydroxychloroquine
- Smoking or chewing tobacco
- Heavy alcohol use
Psoriasis Treatment Options
- Topical medications
- Injections of biological medications
- Oral therapy with immunomodulators and anti-inflammatory medications
- Phototherapy
- Laser treatment
Contact us today at our Bakersfield dermatology office to schedule an appointment for a psoriasis evaluation.

Acne can wreak havoc on your skin, leaving it feeling oily and uncomfortable. Surprisingly, a moisturizer could be the missing piece in your acne care routine. If you’re undergoing any of the following acne treatments, incorporating a moisturizer might be just what your skin needs:
- Benzoyl peroxide
- Salicylic acid
- Adapalene, tazarotene, or tretinoin
- Isotretinoin (a prescription treatment for severe acne)
These treatments are known to dry out and irritate the skin. However, using a moisturizer daily can help your skin better tolerate these medications.
A moisturizer can also be a savior when your skin feels parched, especially during the cold winter months.
Dehydrated skin can trigger an overproduction of oil, which can lead to more breakouts. A well-chosen moisturizer can prevent your skin from becoming excessively dry and irritated.
Why Dermatologists Include Moisturizers in Acne Treatment Plans
So, what type of moisturizer is ideal for someone with acne-prone skin? Look for products with these labels on the container:
- Oil-free
- Non-comedogenic
- Won’t clog pores
When you spot these descriptions, it’s a good sign that the moisturizer is unlikely to exacerbate your acne.
When should you apply moisturizer if you have acne? The rule of thumb is to use it when your skin feels dry. Dermatologists recommend incorporating it into your daily routine, especially after cleansing, as it helps lock in much-needed moisture.
Sealing in Moisture for Healthy Skin
After washing your face, leave some water on your skin before applying moisturizer. This can be a game-changer in maintaining skin hydration.
Now, when can you expect to see results? Studies show that most patients experience a reduction in acne between 4 to 8 weeks after starting to use an acne-friendly moisturizer. These studies typically involve patients following a comprehensive acne treatment plan, including acne medication, cleanser, and moisturizer, all carefully chosen by dermatologists.
If you’re still skeptical about introducing a moisturizer into your acne care routine, it might be time for a chat with a dermatologist. Schedule an appointment and Bakersfield dermatologist Dr. Raskin will provide personalized advice on how to effectively clear your acne and develop a tailored treatment plan.

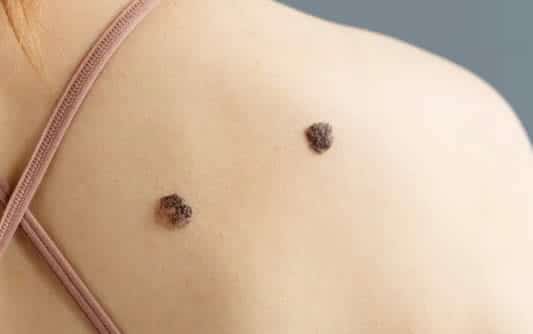
Skin tags, those small flaps of skin that often emerge in areas prone to friction like the neck, underarms, and face, are a common occurrence, with most individuals experiencing at least one during their lifetime.
For those dealing with skin tags, Dr. Raskin, a board-certified dermatologist in Bakersfield provides in-office solutions to safely remove them. Dr. Raskin offers insights into the nature of skin tags and whether they warrant concern.
Understanding the Origins of Skin Tags
Skin tags are benign growths, appearing as small skin bulbs atop stalks. While they can affect anyone, they are more prevalent among middle-aged individuals, both men and women alike.
The exact cause of skin tag formation remains unclear, although they might develop when thicker patches of skin trap clusters of excess collagen and blood vessels. This can stem from friction within skin folds or genetic predisposition to skin tag development.
Factors Contributing to Skin Tag Formation Several factors can increase the likelihood of developing skin tags, including:
- Obesity
- Pregnancy
- Diabetes
- High cholesterol
- Hypertension (high blood pressure)
- Human papillomavirus (HPV) infections
- Hyperinsulinemia (excess insulin levels)
For some individuals, skin tags could potentially signify heightened insulin resistance, atherosclerosis (hardened arteries), polycystic ovary syndrome (PCOS), or cardiovascular issues.
When Skin Tags Pose Problems
Typically, skin tags are harmless and require no removal for health reasons.
However, Dr. Raskin might recommend skin tag removal if they bleed, become entangled with clothing or jewelry, grow excessively, display multiple colors, or cause persistent irritation. Some individuals also opt for removal due to self-consciousness related to the appearance of these growths. Consulting with Dr. Raskin can help determine whether skin tags should be removed.
To arrange a diagnostic evaluation for skin tag removal, contact our dermatology office today to schedule an appointment.

Dealing with atopic dermatitis, commonly known as eczema, is a daily challenge for many individuals. Approximately 30% of the American population grapple with eczema, which can make it difficult to navigate the day and achieve restful sleep while contending with the persistent itching and discomfort it brings. Dr. Michael Raskin, a dermatologist practicing in Bakersfield, wants you to recognize that there are practical strategies to effectively manage this chronic skin condition and regain control over your daily life.
Exploring Diverse Approaches
It’s important to recognize that eczema manifests differently in each person. Adopting a comprehensive approach to minimize the frequency and intensity of symptoms can offer sustained relief. Given that eczema lacks a single causative factor, there isn’t a one-size-fits-all solution. Therefore, it’s advisable to consider a range of strategies to optimize your quality of life despite eczema’s presence.
Identifying Personal Triggers
Eczema often follows a pattern of flare-ups triggered by various environmental factors and substances, including:
- Sun exposure and hot weather
- Excessive sweating
- Irritants like fragrances in lotions, soaps, and perfumes
- Laundry detergents and clothing materials
- Stress
- Allergens and microbes
- Severe cold weather
- Texture of fabrics
Being attuned to specific triggers empowers you to avoid or modify situations to minimize their impact on your condition.
Developing Tailored Approaches
Should you discover a skincare regimen that effectively reduces eczema flare-ups, itching, and irritation, it’s wise to stick to it diligently. Alternatively, if a prescribed medication proves most effective, adhering to the treatment regimen is crucial. Self-care practices contribute significantly to managing and alleviating uncomfortable symptoms.
Cultivating a Positive Mindset
Engaging in relaxation techniques like meditation, yoga, or mindfulness exercises can divert your attention from the itching and irritation of eczema. Guided imagery, in particular, offers a mental escape, proving beneficial, especially if stress exacerbates your symptoms.
Exploring Natural Alternatives
Embracing natural remedies like coconut oil or sunflower oil can provide soothing and moisturizing effects without the irritants present in cosmetic products. Experimenting with such remedies may offer relief from itching and redness. Establishing a routine involving these natural options can become integral to your daily skincare regimen.
While essential oils and aromatherapy might be less suitable due to potential skin irritation, it’s important to note that eczema management isn’t uniform. Finding approaches tailored to your specific condition is key.
If managing eczema symptoms has been a struggle, know that you’re not alone. Reach out to Bakersfield dermatologist Dr. Raskin and schedule an appointment today.

The most severe type of acne is called cystic acne, in which deep and very inflamed acne develops on the face or other parts of the body. The breakouts may be large and can leave unsightly scars. These acne bumps or cysts appear under the surface of the skin and are filled with fluid and often painful.
What causes it?
All types of acne are primarily caused by too many dead skin cells in the pores, overactive oil glands, or a proliferation of acne-causing bacteria. Minor acne blemishes develop when a pore wall breaks near the skin’s surface and leaks infected material into the surrounding area. If a pore wall similarly breaks deeper under the skin’s surface, more severe blemishes can form. If the infected material leaks into adjacent pores, cysts may develop. This most severe kind of acne is usually not related to things like poor cleansing or making poor diet choices. Some people are just more prone to cystic acne than others. It has also been shown to have a genetic element, with parents who had cystic acne more likely to pass severe acne down to their children.
Can it cause scarring?
Because cystic acne damages healthy tissue, it is very common for scars to form in the skin. The best way to limit scarring is to stay on top of treating this type of acne. It is also important to avoid popping or picking at acne cysts, which will likely worsen the breakout and lead to skin damage and scarring. Many patients with this form of severe acne struggle with the embarrassing appearance of breakouts and the lingering effects of scars. This is another reason to get professional treatment from a skilled dermatologist like Dr. Bernard Raskin in Bakersfield.
How is cystic acne treated?
Strong medications are almost always required to adequately treat cystic acne, so seeing a professional is a vital element of treatment. Systemic medications that circulate throughout the body instead of just focusing on one part are a common choice for handling cystic acne. Some of the most frequently prescribed treatments include:
- Oral antibiotics
- Oral contraceptives for women
- Corticosteroid injections
- Accutane
- Surgical skin incision to access and drain the cyst
In can be difficult to gain control of cystic acne, so patients should remember to be persistent and follow the physician’s instructions carefully. Several treatment combinations may be necessary to find the right method for each individual patient. Working closely with your experienced dermatologist is the best way to successfully treat cystic acne.
Schedule an appointment today in our Bakersfield dermatology office.

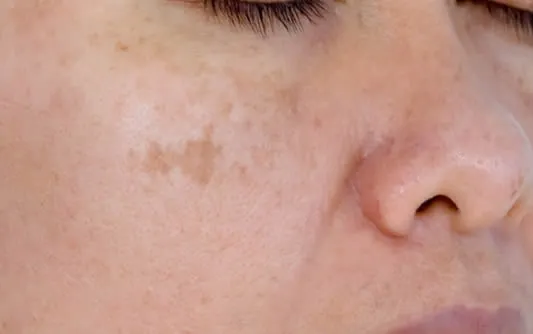
Many people use the terms “age spots” and “sun spots” interchangeably, but they are not the same thing. While both are related to the sun, they have different causes and treatments. In this article, we’ll take a closer look at age spots and sun spots, and how to tell the difference between the two.
What are Age Spots?
Age spots, also known as liver spots, are flat, brown or black spots that appear on the skin as we age. They are usually found on areas of the skin that have been exposed to the sun, such as the face, hands, and arms. Age spots are caused by the overproduction of melanin, the pigment that gives our skin its color.
What are Sun Spots?
Sun spots, also known as solar lentigines, are similar to age spots in appearance, but they are caused by sun exposure. Sun spots are usually lighter in color than age spots, and they can appear anywhere on the body that has been exposed to the sun.
How to Tell the Difference
The easiest way to tell the difference between age spots and sun spots is by their location. Age spots are usually found on areas of the skin that are regularly exposed to the sun, while sun spots can appear anywhere on the body. Additionally, age spots are usually darker in color than sun spots.
Treatment Options
If you are concerned about age spots or sun spots, it is important to see a dermatologist. Dr. Raskin of Bakersfield Dermatology can provide a thorough examination and recommend a treatment plan tailored to your individual needs. Treatment options may include:
- Laser therapy
- Cryotherapy
- Chemical peels
- Topical creams
Prevention
The best way to prevent age spots and sun spots is by protecting your skin from the sun. This includes wearing sunscreen with an SPF of at least 30, wearing protective clothing such as hats and long-sleeved shirts, and seeking shade during the hottest parts of the day. Avoiding tanning beds and other sources of UV radiation is also important.
Conclusion
Age spots and sun spots may look similar, but they have different causes and treatments. If you are concerned about any spots on your skin, it is important to see a dermatologist. Dr. Raskin of Bakersfield Dermatology can provide expert care and treatment options tailored to your individual needs. Remember, prevention is key when it comes to protecting your skin from the sun.
If you are looking for more information about skin cancer prevention and treatment, visit the Bakersfield Dermatology website.

Acanthosis nigricans is a skin condition characterized by dark, velvety patches of skin that usually appear on the neck, armpits, groin, and other skin folds. It can also occur on the hands, elbows, knees, or face. The affected skin can be thick, rough, and sometimes itchy. Acanthosis nigricans can occur in both men and women of any age but is more common in people who are overweight or have insulin resistance or type 2 diabetes.
Causes
Acanthosis nigricans is caused by an increase in insulin levels, which can stimulate the growth of skin cells and increase the production of melanin. This increase in insulin levels can be due to obesity, insulin resistance, type 2 diabetes, hormonal disorders such as polycystic ovary syndrome, or certain medications.
Symptoms
The main symptom of acanthosis nigricans is the appearance of dark, thick, and velvety patches of skin, usually on the neck, armpits, groin, and other skin folds. The affected skin may also have a rough texture or may itch. In some cases, the skin may also have a foul odor.
Types
There are several types of acanthosis nigricans, including:
- Type 1: This type occurs in people with insulin resistance, usually due to obesity or type 2 diabetes.
- Type 2: This type occurs in people who do not have insulin resistance or diabetes but have a genetic predisposition to the condition.
- Drug-induced: This type occurs as a side effect of certain medications, such as hormones, growth factors, or chemotherapy drugs.
Treatment
There is no specific cure for acanthosis nigricans, but treating the underlying cause can improve the condition. For example, losing weight and improving blood sugar control can help improve acanthosis nigricans in people with insulin resistance or type 2 diabetes. In some cases, medications or topical treatments may be prescribed to help reduce the appearance of the patches. Dermabrasion, laser therapy, and chemical peels are also used to improve the appearance of affected skin.
Prevention
Maintaining a healthy weight, exercising regularly, and eating a healthy diet can help prevent the development of acanthosis nigricans. Managing any underlying medical conditions, such as diabetes or hormonal disorders, can also help prevent the condition. If you notice any changes in your skin, especially in the skin folds, consult with Dr. Raskin Bakersfield dermatologist. Early diagnosis and treatment can help prevent the condition from getting worse.

Granulomas are small areas of inflammation in tissues of the body that develop in response to various types of irritants, infections, or foreign substances. They are clusters of immune cells, such as macrophages, that gather together to surround and contain the irritant. Here is a closer look at the causes, symptoms, types, and treatments of granulomas.
Causes
Granulomas can form in response to a variety of factors, including infections, inflammation, autoimmune diseases, and exposure to certain substances. Some of the most common causes of granulomas include:
- Infections such as tuberculosis, fungal infections, and leprosy
- Autoimmune diseases such as sarcoidosis and Crohn’s disease
- Exposure to foreign substances such as talcum powder or silicone
- Chronic inflammation due to conditions such as rheumatoid arthritis or inflammatory bowel disease
Symptoms
The symptoms of granulomas vary depending on the location and cause of the granuloma. In some cases, granulomas may not cause any symptoms at all. However, common symptoms of granulomas include:
- Skin lesions or bumps
- Coughing
- Fatigue
- Shortness of breath
- Weight loss
- Joint pain or stiffness
- Abdominal pain or discomfort
Types of Granulomas
There are several types of granulomas, including:
- Tuberculoid granulomas: These are caused by tuberculosis or other mycobacterial infections and are characterized by a central area of caseation necrosis surrounded by a layer of immune cells.
- Foreign body granulomas: These develop in response to foreign substances that are not able to be broken down by the body, such as talcum powder or silicone.
- Sarcoid granulomas: These are characteristic of sarcoidosis, an autoimmune disease in which immune cells cluster together in the lungs, lymph nodes, and other organs.
- Granulomatous vasculitis: This is an inflammatory condition that affects the blood vessels, causing granulomas to form around the vessel walls.
Treatments
The treatment of granulomas depends on the underlying cause and the severity of symptoms. Some treatment options include:
- Antibiotics or antifungal medication for infections
- Steroid or immunosuppressive medication for autoimmune diseases
- Surgical removal of foreign bodies
- Injections of corticosteroids into the affected area to reduce inflammation and promote healing
In some cases, granulomas may not require treatment and may go away on their own. If you have symptoms of a granuloma, it is important to seek medical attention to determine the underlying cause and appropriate treatment plan. Schedule an appointment with Dr. Raskin today!